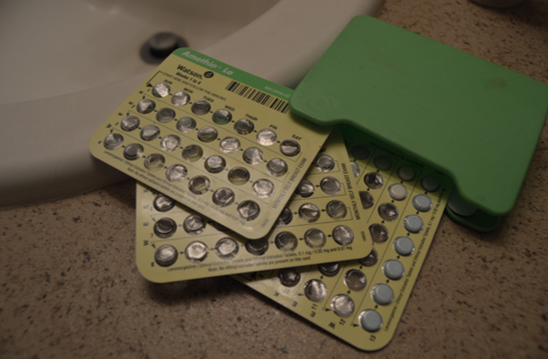
Birth rates between the ages of 15-19 have been decreasing in the United States since 2013 according to the Center of Disease Control and Prevention (CDC). This change has been largely attributed to the availability of birth control to high school and college age students. Although this decrease is viewed as positive, many people report that hormonal birth control has affects their mood negatively. A recent study in Denmark has claimed there is a positive correlation between hormonal birth control and depression.
People take birth control for a myriad of reasons, so they can have sex without getting pregnant, for acne management, to treat menstrual cramps and pain, even to treat moods.
“Over the years, more than a few patients in my women’s health practice have told me that their hormonal birth control — the pill, patch, ring, implant, injection, or IUD — made them feel depressed,” Monique Tello, MD, MPH wrote for Harvard Health Publications. However, a just-published study finally meets the criteria to qualify as high-quality – and therefore believable.
“The study of over a million Danish women over age 14, using hard data like diagnosis codes and prescription records, strongly suggests that there is an increased risk of depression associated with all types of hormonal contraception.”
The study published in Jama Psychiatry claims that teens taking hormonal birth control have an 80% increase risk of taking antidepressants.
Before, it was deemed near impossible to scientifically prove that birth control was the cause of the higher rates of depression, due to other factors such as preexisting conditions and life circumstances, but now there is academic proof to back up what many who take birth control already know to be true.
“The risk of depression has been recognized since women were able to get their hands on oral contraceptives,” National Women’s Health Network executive director Cindy Pearson said about the Danish findings. What’s changed is now there’s data to back up the experience of many women.
“It makes sense biologically,” she says, “and it’s been reported by women for 50 years.”
“I have used three types of birth control since 2015, the pill (pirmella), the injection (depoprovera), and Nuvaring,” alum Madeleine Yount (‘12) said.
“I decided to start birth control to help me with me my mood swings and some of the depressive feelings I was having immediately before the start of my period.”
Yount explained that her doctor was aware of her existing anxiety disorder before she was prescribed birth control. She did feel a change in her mood after starting birth control, but she traveling abroad at the time, so she attributed the depression to the stress.
Yount then decided to try Depoprova (Depo), since it last for three months, and she would not need to remember a pill.
“The first few days of Depo were okay,” Yount recalled. “Then I had terrible mood swings. I wanted to be alone. […] I ostracized my closest friends and cried for no good reason. […] When I called my mom she was scared for me.”
Yount explained that on depo she lost interest in hobbies, gained weight and experienced symptoms similar to Irritable Bowel Syndrome (IBS).
“For me, every day was a challenge and I began to get used to it,” Yount said. “I did not see myself anymore. […] Because I was so accustomed to my own erratic behavior, I did not know what my “normal” was.”
When Younts symptoms started to include hair loss and an inability to eat, she got off Depo and got on Nuvaring.
Yount improved. Nuvaring, unlike other birth control, is concentrated hormones, so it does not affect the body for as long.
“Now that I am on my third month of Nuvaring, I still have anxiety and depressive thoughts,” Yount said. “But I know when they will be and can mentally prepare for them. […] Nuvaring is not ideal, and I have some other side effects, but holy hell when I look back at who I was even a few months ago I don’t recognize the person I was.”
New College students expressed that they would of liked to have had their doctors be more informative in terms of the effects of hormonal birth control.
The issue with conclusively citing that birth control was the cause of depression is that people who take birth control do not exist in a bubble. So, claiming that birth control was the truly affecting mood was complicated by other events in people’s lives.
“Lo Estrin made me seriously depressed, and I think that really effected my first year of college,” thesis student Cayli Caruso said.
Caruso stated that she was on the birth control for a year, and it affected her mood very negatively. She got off of it and transferred from University of Central Florida to New College and her mood improved.
“There wasn’t really a conversation about side effects with the gynecologist,” Caruso said. “I looked up [the possible effects] of birth control online and that’s how I found the answer.”
“Thing I found most true from changing [birth control] brands all the time, is that all of them are going to affect your mood in some way,” Caruso said. “Now that I am off of birth control, this is the first time in four years I have been clear headed.”
Caruso originally began birth control to treat heavy menstruation. She is nervous to not be on birth control at all, but is glad to be feeling better.
Since birth rates have been decreasing, the reasons why doctors might be less forthright with negative side effects make sense, but for those who have mental illness, it is important to know how medications could affect them.
“My doctor really minimized the interaction between birth control and mental health,” thesis student Melissa Rettig said. “But people I knew who worked at Planned Parenthood cautioned me about taking hormonal birth control in regards to my depression.”
Although she suffers from depression, Rettig did not claim that hormonal birth control was not an option. Rettig explained that at first, she did suffer from mood problems relating to birth control, but she experimented with different methods and made it work for her. She tried both Lo Estrin and Nuva Ring, but eventually returned to Lo Estrin.
“What I hope is that see access to education about reproductive health in general,” Rettig said. “With education and greater access to resources, more people with uteruses will be able to make informed choices about what kind of health care is best for them.”
The study on the Danish women adds clout to the experiences of many people on birth control and will hopefully encourage doctors to be more open with their patients about potential side effects.
“This fits into a long history in which the experiences of all kind of women, but especially brown, black and poor women, have been de-legitimized,” Rettig added. “I think that the fact that we have to have this empirical evidence to back up how women actually feel is ridiculous.”
The empirical evidence proves what many people on hormonal birth control have been claiming all along.
http://www.health.harvard.edu/blog/can-hormonal-birth-control-trigger-depression-2016101710514
Skovlund CW, Mørch LS, Kessing LV, Lidegaard Ø. Association of Hormonal Contraception With Depression. JAMA Psychiatry. Published online September 28, 2016. doi:10.1001/jamapsychiatry.2016.2387