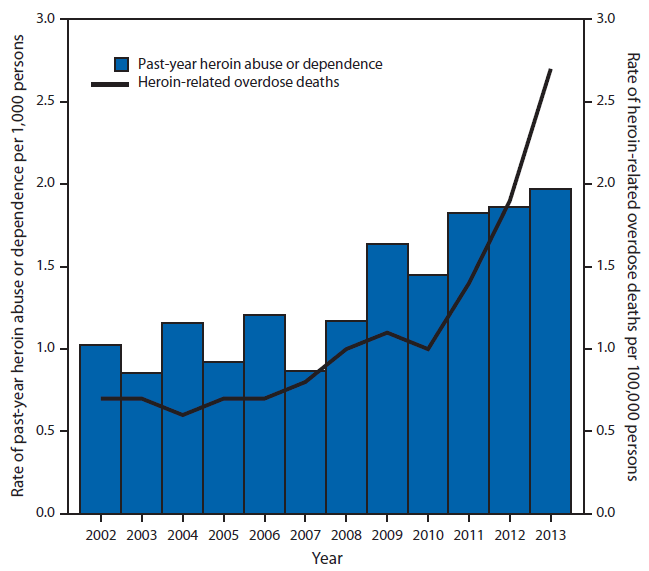
Heroin use has increased dramatically in the U.S. over the past decade. Between 2006 and 2013, a study by the Substance Abuse and Mental Health Services Administration (SAMHSA) revealed that the number of first-time heroin users doubled from 90,000 to 169,000.
Health care providers wrote more than 250 million prescriptions for painkillers last year, according to federal data published by the New York Times – enough for every adult in America to have a bottle.
Racial disparities in drug policy
The crack-cocaine epidemic of the 80s and 90s has been replaced with an even more deadly drug of choice, opiates, and yet the response from law enforcement and government agencies has been the rejection of the zero-tolerance polices and sky-rocketing incarceration rates that have defined drug policy in the U.S. for almost a century.
This movement toward compassionate care centers around the treatment of addiction as a disease – not as a criminality issue – with a focus on rehabilitation as opposed to punitive action. This approach has been scientifically and socially proven to be the best course of action for dealing with drug abuse, as evidenced by the growing number of countries who have implemented harm reduction and decriminalization policies, including Canada, Portugal and Switzerland. But the changes have come far too late to benefit the millions of people of color who were forced behind bars or into the streets as a result of the “Just Say No” campaign.
According to a study published in the New York Times, nearly 90 percent of those who tried heroin for the first time in the last decade were white. This shift in demographics has been directly linked to the shift toward harm reduction policies and decreased incarceration rates. White parents are more likely to have the resources to fight back when their kids are arrested for drug possession or use and can afford to send their children to court-ordered rehab facilities instead of prison.
Marc Mauer, the executive director of The Sentencing Project, a group that targets racial disparities in the criminal-justice system, said this in an interview on racial disparity and drug policy with The Atlantic: “The response to the rise in heroin use follows patterns we’ve seen over decades of drug scares. When the perception of the user population is primarily people of color, then the response is to demonize and punish. When it’s white, then we search for answers.”
This response has been documented in U.S. drug policy since the reactionary cries of “reefer madness” dominated the 1930s. Harry Anslinger, the forefather of the War on Drugs and marijuana prohibition, served as first commissioner of the Federal Bureau of Narcotics, the predecessor to the DEA, for 32 years. The rationale behind his criminalization of marijuana and the non-psychoactive hemp plant is as follows:
“There are 100,000 total marijuana smokers in the U.S., and most are Negroes, Hispanics, [and] Filipinos.”
Ronald Reagan cited Anslinger’s policies as the basis for his expansion of the War on Drugs in the 1980s.
Sarasota County
Sergeant Donny Kennard, head of the Sarasota County Sherriff’s Pharmaceutical Diversion Unit, reported that since June 2015 there have been 64 nonfatal and 8 fatal overdoses in Sarasota County. July was the Sarasota Sherriff’s office “worst month” – officers responded to 24 overdose calls.
“So far, the overdoses in 2016 are significantly down from last year,” Kennard said. Reports indicate one fatal and seven nonfatal opiate-related overdoses so far this year.
In 2015, Manatee was Florida’s number one county in terms of heroin addiction, overdoses and deaths. Bradenton has seen a 65 percent decrease in 911 calls for heroin overdoses in 2016, with zero heroin overdose deaths.
The sheriff’s department partially attributed this decrease to a recent drug bust in the Bradenton area. The bust was a joint effort between the Sarasota County Sherriff’s Office, Bradenton County Sherriff and the Drug Enforcement Agency (DEA). Fifteen people were arrested as part of an 18-month-long operation.
According to The Bradenton Times, authorities confiscated about 3.5 kilograms of heroin, at an estimated street value of $262,500; 3 kilograms of cocaine with a street value of $111,000; 200 grams of fentanyl; 100 hydromorphone pills; 28 guns; and more than $327,000 in cash and assets. The fentanyl and hydromorphone were presumably used to cut the heroin, increasing its potency and its profitability – along with its potential to kill. Fentanyl is 80 to 100 times more powerful than morphine, and when mixed with other opiates such as heroin, the synergistic reaction is often deadly.
Between 2005 and 2007, more than 1,000 U.S. deaths were caused by fentanyl-heroin overdoses, according to the Drug Enforcement Administration. Seizures of drugs containing the painkiller jumped from 942 to 3,334 between 2013 and 2014.
Naloxone
Harm reduction, a public health policy that deals with reducing the negative consequences of drug use, encourages accessibility to supervised injection facilities and opioid antagonists such as naloxone.
The Sarasota County Sherriff Department is now equipped with EVZIO, a single-use naloxone auto-injector that can reverse an overdose almost immediately. Since they received the medicine – at zero cost due to a grant from the pharmaceutical company – there have been two deployments, both of which resulted in full-recoveries.
The department also has access to heroin overdose toolkits provided by SAMHSA, a branch of the U.S. Department of Health and Human Services. These toolkits contain information about opiate use and abuse, overdose prevention, naloxone administration, and what to do if someone around you is overdosing.
Increased availability of these harm reducing measures are becoming more important in the discussion of public health polices. Advocates of harm reduction say the U.S. can no longer afford to ignore such potentially life-saving measures. Deaths from heroin overdoses nearly quadrupled from 2002 to 2013, the Center for Disease Control and Prevention (CDC) reported, with more than 47,000 drug overdose deaths in 2014.
Supervised Injection Facilities
Supervised injection facilities are medically supervised facilities where individuals who use intravenous drugs can inject pre-obtained drugs – without fear of legal ramifications. They have been proven to reduce the risks of injection-related injuries, death from overdose, vein damage, and the transmission of blood-borne diseases such as HIV/AIDS and Hepatitis.
The facilities provide sterile needles, factual information about drugs and basic health care, treatment referrals, and access to medical staff. Some facilities also offer counseling intended to assist individuals who may not have the means to seek treatment on their own. No supervised injection facilities currently exist in the United States.
The Canadian Medical Association Journal estimates that as of 2009, there were 65 safe injection facilities operating in 27 cities in eight countries.
Opioid Replacement Therapy
Along with the promotion of supervised injection facilities, harm reduction policies advocate for the increased availability of opioid replacement therapy (ORT) as a means to treat opioid addiction and dependence.
The National Institute on Drug Abuse estimates “that between 26.4 million and 36 million people abuse opioids worldwide, with an estimated 2.1 million people in the United States suffering from substance use disorders related to prescription opioid pain relievers in 2012, and an estimated 467,000 addicted to heroin. The number of unintentional overdose deaths from prescription pain relievers has soared in the United States, more than quadrupling since 1999. There is also growing evidence to suggest a relationship between increased non-medical use of opioid analgesics and heroin abuse in the United States.”
Opioid replacement therapy consists of supplying addicts with longer-acting, less euphoric opioids such as methadone or buprenorphine in place of their usual drug of choice, under the supervision of medical professionals. The primary aim of ORT is to reduce the symptoms of drug withdrawal and the intensity of drug cravings. Unlike alcohol or benzodiazepine withdrawals, opioid withdrawal rarely results in death, but the process is still extremely uncomfortable and includes nausea, hot and cold sweats, insomnia, muscle cramping, vomiting, irritability, agitation and anxiety.
“The Center for Disease Control and Prevention, the Institute of Medicine, the Substance Abuse and Mental Health Service Administration, the National Institute on Drug Abuse, the World Health Organization and over four decades of government-funded, peer-reviewed medical research unequivocally and repeatedly proven that replacement therapies like methadone maintenance are the most effective treatments for opioid dependence,” the DPA reports.
Sidebar:
Treatments for opioid addiction
Methadone: Opioid. Habit-forming. Controlled substance. Taken at specially licensed clinics. Daily pill. Cost: About $150 per month.
Buprenorphine: Opioid. Habit-forming. Controlled substance. Must be prescribed by doctor who receives a DEA waiver. Pill often taken every other day. Cost: About $300 per month (generic).
Buprenorphine/naloxone (Suboxone): Daily film placed under tongue. Habit-forming. Controlled substance. Must be prescribed. Requires DEA waiver. Cost: About $450 per month.
Naltrexone shot (Vivitrol): Opioid blocker. Not habit-forming. Non-controlled. Must be prescribed. Does not require waiver or registration with DEA. Monthly injection. Cost: About $1,000 per month.
Sources for costs: Drugs.com; Darius Rastegar; Johns Hopkins School of Medicine; Alkermes
Information for this article was taken from washingtonpost.com, nytimes.com, Bradenton.com, theatlantic.com